By Andy Ford, biomedical scientist and Unite member
The decision from the UK National Screening Committee not to offer prostate cancer screening to high-risk men once again shows the hollow nature of the Starmer government’s commitment to “prevention over treatment”. One in eight men will be affected by prostate cancer, with around 12,000 deaths a year.
The PSA (Prostate-Specific Antigen) test can be a simple add-on to any blood test, and It is hard not to see the hidden hand of the Treasury in the decision not to widen out its use. One man every 45 minutes is diagnosed with prostate cancer, and half of them are diagnosed late, after presenting with symptoms. For many, at that point, it is too late.
Treatment for late presenting prostate cancer – hormone therapy, radiotherapy, chemo – is far more invasive and damaging than the treatments used in early diagnosis. It is also a lot more expensive.
And yet the Committee has said “no” to screening, even for those at higher risk, such as Black men or those with a family history of the disease. They advocate screening only those men with a specific risky genetic mutation.
They say that screening risks “over-diagnosis and over-treatment”. They talk about too many false PSA positives, too many biopsies, too much damage – all for nothing. That was only true in the 1990s.
Sweden, Norway and Germany have moved on from screening and then biopsy with all their side effects. They escalate to non-invasive scans using MRI for men with a positive PSA test, followed by a complex process of risk analysis and statistical analysis, before going in with a biopsy.
A proper risk-based screening programme would cost around £25 million a year, but would save thousands of lives. Avoiding even 20% of late diagnoses would also save a lot, even leaving aside the huge emotional impacts on patients and their families.
According to the charity Prostate Cancer UK, a five-year targeted screening programme would show a net financial benefit of £54 million by reducing treatment costs and by gains in quality of life. Late-stage treatment costs on average £127,000 per patient, as against £13,000 for early stage.
And yet…the decision, which is subject to review, seems to prioritise savings in this current year over much bigger savings, in money and lives saved, in future years.
You are left with the feeling that “prevention over treatment” is more of a government excuse for flatlining hospital budgets than a real strategy of prevention. We saw exactly the same thing earlier this year with weight loss drugs
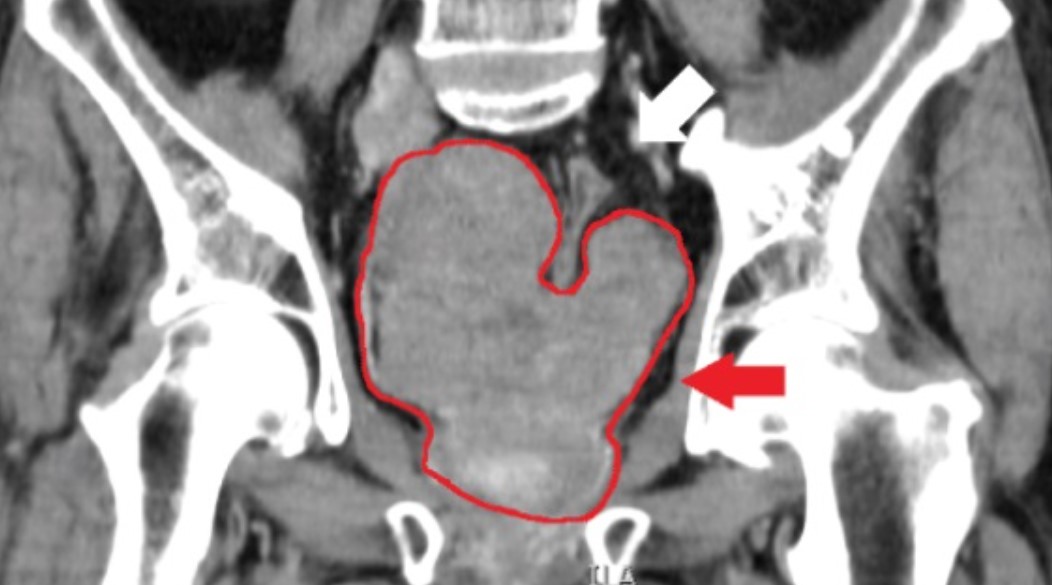
[Feature picture showing a CT scan of a prostate is from Wikimedia Commons, here]